CASE REPORT
Loco-Regional BCGitis Revealing a HIV Infection in an Infant: A Case Report
Ibtissam Khattou*, Ouidad Louachama, Noureddine Rada, Ghizlane Draiss, Mohammed Bouskraoui
Article Information
Identifiers and Pagination:
Year: 2019Volume: 11
First Page: 13
Last Page: 16
Publisher ID: TOIDJ-11-13
DOI: 10.2174/1874279301911010013
Article History:
Received Date: 21/10/2018Revision Received Date: 20/01/2019
Acceptance Date: 02/03/2019
Electronic publication date: 28/03/2019
Collection year: 2019

open-access license: This is an open access article distributed under the terms of the Creative Commons Attribution 4.0 International Public License (CC-BY 4.0), a copy of which is available at: (https://creativecommons.org/licenses/by/4.0/legalcode). This license permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
The BCG disease is a specific complication of the Bacille Calmette and Guerin (BCG) vaccine. It is often in the form of benign local BCGitis, however the BCGosis is a lethal disseminated disease that can occur in a patient with immunodeficiency. The prognosis depends on the immune status of the patient, and the quality of management. Therapeutic modalities are very controversial. In this article, the authors report a case of loco-regional BCGitis revealing an HIV infection.
1. BACKGROUND
Bacille Calmette and Guerin (BCG) is the only vaccine used since 1921 to protect against tuberculosis. It is a live vaccine, derived from Mycobacterium bovis, which has been attenuated in vitro. It confers protection of the order of 80% against miliary tuberculosis and tuberculous meningitis [1]. However, the BCG disease is a rare and specific complication, often benign in an immunocompetent patient but it can be serious in immunodepressed and whose therapeutic protocols are very controversial [2]. We report a case of locoregional BCGitis revealing a retroviral infection (HIV) in the department of pediatric in Mohammed VI University Hospital of Marrakech in Morocco.
2. CASE REPORT
This is a case study of a 10-months-old infant, from non-consanguineous marriage, second of two siblings, of a low socio-economic status, born at term, with normal birth weight. Vaccination was updated and the BCG vaccine was performed at 20 days of age in the deltoid of the left arm. He was admitted for chronic diarrhea for three months. The clinical examination found a nonfebrile child, dehydrated, undernourished with normal cardiorespiratory parameters, and a failure to thrive, oral candidiasis and purulent otitis. The initial investigations showed in hemogram: Hemoglobin: 9.9 g/dl (normal: 10.5-13.5), MCV: 89.5fl (normal), MCH: 28.1 pg (normal), leukocytes: 5 500/uL (normal), neutrophils: 2630/uL, lymphocytes: 2060/uL, Platelets:170.000/uL (normal), and C reactive protein: 0.31 mg/l (normal); his serum electrolytes were within the normal reference range, low cholesterol level: 0.93 g/l, hypoalbuminemia: 27 g/l.Anti-tissue transglutaminase antibodies (ATTG): Negatives. copro parasitological examination of stool was negative.
Initial management included rehydration, nutritional rehabilitation and antibiotic therapy with metronidazole and third-generation cephalosporin. Thereafter the patient presented a urinary tract infection caused by multi-drug resistant Klebsiella pneumonia treated with colistin and amikacin, with bilateral pneumonia (Fig. 1) not responding to antibiotic treatment, and a left axillary adenitis, measuring 4cm / 3cm (Fig. 2) with purulent ulceration of the BCG scar (Fig. 3) Mycobacterium was not detected by smear microscopy and Gene xpert. The histological study of lymph nodes found a loss of follicular architecture, the ultrasound examination objectified a cluster of left axillary lymphadenopathy, so a BCGitis was retained. Therefore, the recurrent infections and loco-regional BCGitis made us suspected about immunodeficiency. At the time, HIV serology was positive (An ELISA test, Confirmed by the Wesrern Blot) with a low level of CD4: 214 cells / mm3 and high level of viral load at 6135907 copies/ml. Co-trimoxazole therapy was initiated followed by rifampicin, isoniazid, pyrazinamide and ethambutol with the application of local isoniazid powder. Three weeks later, antiretroviral therapy was introduced to prevent immune reconstitution inflammatory syndrome (IRIS); the HAART was commenced with 2NRTIs (nucleoside reverse transcriptase inhibitors) associated to PIs (protease inhibitors). He completed nine months of antituberculous therapy with a good outcome (Fig. 4), and the CD4 count: 1050 cells / mm3 and the viral load at 40 copies / ml.
 |
Fig. (1). Bilateral alveolar syndrome, bilateral pneumonia. |
 |
Fig. (2). The left axillary adenitis 4cm/3cm. |
 |
Fig. (3). Purulent ulceration of the BCG scar. |
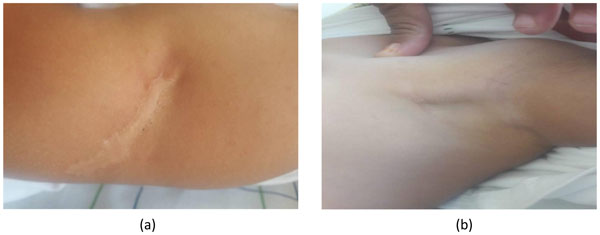 |
Fig. (4). (a) good outcome of ulceration of the BCG scar (b) good evolution of left axillary adenitis. |
3. DISCUSSION
BCG vaccine consists of a live attenuated strain of Mycobacterium bovis, It is harmless in most children. Its protective effect has been estimated in several studies between zero and 80% [3]. Complications of BCG are generally benign in immunocompetent individuals, which are most often due to technical errors of vaccination. On the other hand, in an immunocompromised subject, these reactions are often severe, sometimes even fatal [2].The BCG diseases (BCGitis or BCGosis) are distinguished by the normal reaction of BCG basen on their morphological and evolutionary differences. They must also be distinguished from local pyogenic abscesses with reactive adenitis whose onset is shorter and shows good outcome with antibiotherapy [2]. There are four categories of BCG disease according to their location in relation to the BCG scar: local, regional, distant BCGitis and disseminated or BCGosis [2]. The diagnosis of disseminated BCGitis requires the search for immunodeficiency. This may be a “classic” immune deficiency, as it may be a defect in the IL-12/23 and IFN- γ pathways (Mendelian Susceptibility to Mycobacterial Disease) [4-6]. In our case report, the BCGitis was loco-regional: the occurrence of purulent ulceration at the BCG scar and ipsilateral axillary adenitis without other localizations especially without hepatomegaly and splenomegaly. The history of recurrent otitis, oral candidiasis, chronic diarrhea, and failure to thrive has made us think of immune deficiency. The treatment of the BCGitis is not codified [7]. Some require primary surveillance, while others require antituberculous therapy from the start [8]. For local BCGitis, some teams recommend oral isoniazid or local powder, but without controlled studies. Therapeutic aspiration is indicated in suppurative adenitis or local abscess more than 3 cm. In case of failure or fistulization, surgical excision should be discussed [9]. In distant BCGitis, antituberculous therapy is essential but there is no consensual treatment. Hesseling et al. recommended a treatment with a quadruple combinational antituberculous therapy [10].In an immunocompromised patient, antibacillary treatment is always recommended with quadruple combinational at least for 9 months [10]. The introduction of highly active antiretroviral therapy in HIV-infected individuals is essential [10]. In our case report, the BCGitis was treated with quadruple combinational for 9 months in addition to local treatment with isoniazid powder; three weeks later, the antiretroviral therapy was commenced because the risk of IRIS was high. 3 years later, the outcome was favorable.
CONCLUSION
In this case report, we highlighted the importance of seeking immunodeficiency in the presence of disseminated BCGitis or severe axillary adenitis associated with general signs, secondary to BCG vaccination.
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
Not applicable.
HUMAN AND ANIMAL RIGHTS
No animals/humans were used for studies that are basis of this research.
STANDARDS OF REPORTING
CARE guidelines and methodology were followed to conduct the case study.
CONSENT FOR PUBLICATION
Informed consent was abtained from parents of patient prior to publication.
CONFLICT OF INTEREST
The authors declare no conflict of interest, financial or otherwise.
ACKNOWLEDGEMENTS
Declared none.









